Fight Against Polio
The disease can be eradicated by 2018—with sufficient funds, commitment, and resolve.
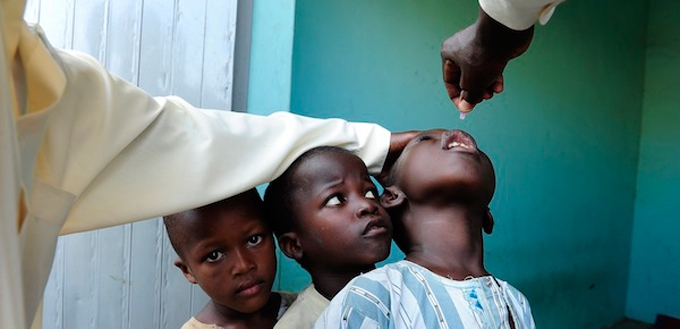
Children receiving polio vaccine drops, Kano, Nigeria, Aug. 5, 2010. Mary F. Calvert/ZumaPress/Corbis
Although no one knows exactly how long polio has been around, malformed bones of Egyptian mummies and stone carvings from around 1400 BCE suggest the disease has dwelled among human populations for thousands of years.
The great irony about polio is that, while it was probably more prevalent in Pharaonic times, it only became a terrifying epidemic in ours. One reason offered by scientists is that in ancient times, infants were protected by maternal antibodies and likely developed lifelong immunity. But as hygiene improved in a rapidly modernizing world, people weren’t exposed to the virus until later in life, when they were no longer protected by their mother’s immune system. Although the introduction of polio vaccines in the mid-twentieth century quickly stalled major polio outbreaks in wealthier countries, it remained endemic in many parts of the world as late as 1988. That year, the World Health Assembly (WHA), the decision-making body of the World Health Organization (WHO), passed a resolution supporting the global eradication of polio. At the time, the virus was still circulating in 125 countries, where it paralyzed 1,000 people a day—filling parents with terror and hospital wards with children who, in many cases, would never walk again.
Within eight years of the WHA declaration, polio cases worldwide dropped almost 90 percent. In 2006, Egypt and Niger were declared polio-free. Last year, India was declared polio-free as well, demonstrating success is possible even in the most difficult circumstances. These accomplishments are part of a steep decline in remaining cases worldwide; there were fewer than 250 new cases reported in 2012. Today, we are seeing the fewest number of polio cases in the fewest countries ever. We have almost succeeded at wiping the virus off the face of the earth.
But “almost” is not good enough. Polio is a stubborn, highly-contagious disease that is easily transmitted as people move across borders, as they do frequently today. In 2006, people living in thirteen countries that had already achieved polio-free status became infected by travelers from the handful of countries where the disease remains endemic. These importations led to large polio outbreaks in several countries, including Indonesia, Somalia, and Yemen.
The latest evidence of polio’s propensity for travel turned up in sewage samples collected last December at two different sites in Cairo. Polioviruses detected in these samples were found to be closely related to the poliovirus circulating in Pakistan.
Although no new cases of polio have been reported in Egypt since 2004, the Ministry of Health and Population quickly geared up to conduct mass polio vaccination campaigns to ensure high immunity levels. Within four months after the virus samples were confirmed, fifteen million children under age five will be protected.
This recent discovery of the poliovirus samples in Cairo underscores the difficulty—and the urgency—of the global effort to eradicate polio. Until the poliovirus is completely eradicated everywhere, no country is safe from reinfection. It also reminds us of the incredible power of vaccines to solve some of the world’s biggest health problems.
The smallpox vaccine is one of the most impressive examples of what the world can achieve with life-saving vaccines when backed by political commitment and public will. As recently as 1967, the WHO estimated that ten to fifteen million people a year were contracting the disease, two million died, and millions more who survived were left disfigured or blind. After thirteen years of dedicated vaccine campaigns, smallpox was completely eradicated—the first successful global vaccination effort.
Vaccines have reduced the number of children dying from diphtheria by 93 percent, cut child deaths from tetanus by 85 percent, and lowered measles deaths by 74 percent. In Sub-Saharan Africa, more than 100 million young people have received the new MenAfriVac vaccine. It is the first vaccine created specifically to address a disease in the developing world, and it is putting a fast end to the dreaded Meningitis A epidemics that have, for more than a century, left death and devastation in their wake.
Vaccines are an especially important tool in reducing the burden of disease, which takes such a disproportionately heavy toll on developing countries. The problem of global health inequity became visible to me about fifteen years ago, when my wife, Melinda, and I saw a chart in the newspaper breaking down the major causes of death among children. One of the largest sources was something called rotavirus. It was killing 500,000 children a year, yet neither Melinda nor I had ever heard of it. As I quickly learned, rotavirus is the leading cause of diarrhea and it’s preventable with a vaccine that only children in rich countries were getting.
This realization is what prompted both of us to decide to focus on global health and to do everything we could to get the rotavirus vaccine out to every child who needs it. Now, twelve of the world’s poorest countries are giving the rotavirus vaccine to children. By 2015, the number is scheduled to climb to forty countries.
The simple fact is, vaccines work wonders. They prevent disease from striking, which is more efficient and effective than treatment after the fact. They are also relatively cheap and easy to deliver. Yet millions and millions of children—more often in poor countries—don’t get them.
Innovative Collaboration
Before we started the Bill & Melinda Gates Foundation, we assumed that all the obvious steps were already being taken to protect children from vaccine-preventable diseases. But in fact, our first big health initiative was devoted to delivering basic vaccines, because even that is not a simple matter. It’s extraordinarily difficult. Nevertheless, universal coverage with today’s vaccines is achievable. And it is possible that new vaccines will be developed in the future for diseases such as malaria.
To achieve both of these goals would save millions of lives, and they are a major focus of our foundation and the work we are doing with partners such as the Islamic Development Bank (IDB) and His Highness General Sheikh Mohamed bin Zayed Al-Nahyan, crown prince of Abu Dhabi, as well as leaders in other Middle Eastern and Islamic countries.
In 2011, Sheikh Mohamed committed $50 million to polio eradication and vaccine delivery. Last fall, the IDB, a new donor to the polio eradication effort, announced an innovative $227 million financing package to Pakistan that will cover the majority of the country’s polio vaccination campaign costs. It also announced a $3 million grant for polio eradication activities in Afghanistan.
This kind of innovative collaboration between traditional donors, rapidly-developing countries, and emerging economies can take us closer to ending polio and reaching all children, no matter where they live, with the vaccines they need. Another is the Global Vaccine Summit that is taking place in Abu Dhabi in April this year. Under the patronage of Sheikh Mohamed, the summit will unite the world in reaffirming support for the Decade of Vaccines, a commitment endorsed at the World Health Assembly in May 2012 to save more than twenty million lives by 2020. The Global Vaccine Summit also will underscore the importance of building and maintaining effective routine immunization systems to keep all children healthy, no matter where they live.
One of the most incredible examples of the power of vaccines is how close we are to declaring the world polio-free. Fully funding the Global Polio Eradication Initiative’s strategic plan is a critical step in achieving this historic goal, and will help us reach mothers and children with other life-saving vaccines and important health services. Vaccines can protect children for a lifetime, but reaching all children will take a sustained effort. It is this tension, between how much the world has achieved and how much is left to achieve, that causes me to be both optimistic and impatient—an impatient optimist. And polio is the subject about which I am most impatient—and the most optimistic.
Because we have successfully eradicated polio from most countries, many people believe it is a disease of the past, and no longer a risk. As a result, it is sometimes difficult for donors in developed countries to understand why their continued support is so important.
But in fact, polio still strikes and paralyzes children today. Until it’s eradicated everywhere, it remains a risk everywhere. And getting to that remaining 1 percent is much harder than anyone ever imagined. The best way to illustrate the challenge we still face with polio is to compare it to what it took to stamp out smallpox worldwide.
With smallpox, every individual infected with the virus got an unmistakable rash on the skin. As soon as someone saw a new case, vaccinators moved aggressively into nearby towns to “ringfence” and contain the virus. Once immunized, people never needed another smallpox vaccination.
Polio, on the other hand, is transmitted silently and just 1 percent of infected people show symptoms. The other 99 percent are contagious without knowing it. When symptoms do appear, they may not be definitive. Symptoms often start with a fever and headache. A few days later, ordinary muscle aches may get increasingly severe and the patient’s reflexes can start to slow down. Only then does paralysis sets in. But, even when a health worker sees a child with paralysis, it takes another two weeks to collect and analyze stool samples. By the time a diagnosis is confirmed, the poliovirus may have traveled hundreds of miles in any direction.
To create an effective “population immunity,” polio vaccinators must reach at least 80 percent of the population, sometimes as much as 95 percent, depending on a number of factors. Achieving 95 percent coverage is very difficult, even in wealthy countries. It is far more challenging in the developing world.
Take the example of India, the most recent country to eliminate polio. India started with the same approach as the United Kingdom: vaccinating children when they came into the clinic for routine visits. But too many Indian children never see the inside of a clinic, so the Indian government added a supply-side approach to the demand-side approach. That is they started going out into communities, finding children, and vaccinating them house by house.
Think about what this requires. India has more than a billion people. Geographically, it is three times larger than Egypt. It also features some of the most severe terrain and weather in the world. During a flood in 2007, for instance, health workers in Bihar state had to walk for miles in water up to their waists to vaccinate children living in a remote area along the Kosi River. Not only did they have to carry the vaccines in a box on their head to keep it out of the water, they also had to keep the vaccines cold the whole time. Similar efforts of courage and commitment happened over and over, since every child has to be vaccinated three or more times to ensure full immunity.
India’s polio program employed two million people and was almost entirely paid for by the Indian government, which speaks volumes about the political commitment that went into the program. Its accomplishment of wiping polio out of the country is the most impressive global health success I’ve ever seen.
A Moral Quest
The challenges in the remaining three endemic countries—Afghanistan, Pakistan, and Nigeria—are just as daunting, though for different reasons.
In Nigeria, a decade ago, some leaders in the northern part of the country started the rumor that the polio vaccine reduced fertility in the children who received it. Campaigns were suspended for a year while officials disproved the allegations. A large epidemic sliced through Northern Nigeria, and polio spread back into about twenty nearby countries where it had been eliminated. All those countries had to ramp up again to win the fight for the second time. The rumors persisted even after the campaigns were restarted, and to this day some parents refuse to let their children be vaccinated.
In Afghanistan and Pakistan, militants in some areas won’t give vaccinators access to local children. Even in the places where vaccinators can go, there is no guarantee that they will be safe.
Not surprisingly, when I lay out these facts, people usually ask me two questions. First, given all the challenges, is complete eradication of polio really possible? And secondly, should we bother putting in the work it’s going to take?
My answer to both is yes. We can eradicate polio, and we should. Why? In a word, because of innovation.
Consider the long history of the disease. Though it’s been around for thousands of years, we only figured out that it is contagious 200 years ago. It was just one hundred years ago that we learned it is a virus. Fifty years ago, we developed the vaccine to prevent it. Twenty-five years ago, the world resolved to eradicate it. At each step along the way, a breakthrough—in medical knowledge, diagnosis and treatment technology, global collaboration, and delivery—changed how we think about the problem.
New innovations are continuing to help us overcome remaining obstacles to eradication. In the past year, Nigeria started using a new technology to solve an old problem: How do you vaccinate every child when you don’t know how many there are?
The polio program uses what they call “microplans” to assign routes to vaccinators, with the goal of covering every part of the country. Previously, the maps weren’t accurate or detailed enough to drive universal coverage. Thousands of settlements were simply overlooked. Distances could be off by many miles, meaning that what the microplan said was a twenty-mile trip and a day’s worth of work might end up being a forty-mile trip and two days-worth.
Recent innovations in mapping technology have enabled polio teams to identify areas that vaccinators previously missed. The question is no longer, “How many children are there and where might we find them?” It is now, “How do we most efficiently vaccinate every child?”
Innovations like this are the inspiration for my optimism. But to make sure innovation in technology transforms our world in positive ways, human beings need to point it in the right direction. That takes public will, as seen in people, organizations, and their governments coming together to drive polio into extinction.
Many organizations helped push the eradication resolution through the World Health Assembly, but the one you wouldn’t expect is Rotary International. Rotary is a service organization with 1.2 million members who live in almost every country in the world.
While Rotarians pledge to put service above self, they have no specific global health mandate. They are neither polio experts, nor policy leaders. But they are regular people who go to work and spend time with their families. For three decades, they have also spent time advocating for polio eradication, raising money to support vaccination, and giving kids all over the world polio drops.
Other partners include the Centers for Disease Control, UNICEF, and the WHO. We rely on them to advance polio eradication, but that is still not enough. We also need people whose jobs have nothing to do with the health of poor people to act. That is public will in the face of global health inequity.
I see strong commitment from leaders in all three endemic countries. When I went to Nigeria for the first time four years ago, I met with two groups of leaders: the religious leaders in the north, who are in the best position to encourage anxious parents to vaccinate their children, and the state governors, who have the power to hold the health system accountable for results. At the end of our two-hour meeting, the governors signed a document committing them to the goal of eradication and spelling out their personal obligations.
Last September, I went to New York to attend a United Nations polio meeting. Nigerian President Goodluck Jonathan, Afghanistan President Hamid Karzai, and Pakistan President Asif Ali Zardari all came to talk about their commitment to eradication. Their presence, as much as the content of their remarks, showed that the initiative has unprecedented momentum.
It’s important for wealthier country governments to be involved and generous with their aid as well. The proof of great leadership is the ability to be long-sighted and keep the big picture in mind. A number of donor governments have decided to prioritize foreign aid, even in the face of great financial challenges, which is exactly the kind of commitment I’m speaking of.
That leaves the second question to answer: Why is it worth it? Polio doesn’t kill anywhere near as many people as AIDS, tuberculosis, malaria, or rotavirus, so why should the world focus on eradicating it?
First, there is no such thing as keeping polio at its current, low levels. We have gotten to this point because of our shared commitment to work together until the job is done. Vaccinators are wading through flooded rivers, developing-country governments are investing scarce resources, and the global health community is on high alert. These are not sustainable approaches, but they are what is required if we are to be successful. If we don’t keep investing, cases will shoot back up to the tens of thousands annually in dozens of countries—precisely at a moment when we are at the brink of seeing polio go into extinction.
Secondly, successfully eradicating polio will generate lessons that benefit all of global health. We are on the verge of doing something we’ve never been able to do before—reaching the vast majority of children in the remotest places in the world to help secure their health and future. We are building systems, developing technology, and training workers that make it possible to help people who have never received any help. When polio is gone, we can use the same systems, technology, and people to deliver other lifesaving solutions, especially routine vaccinations for diseases like rotavirus and measles.
These are practical arguments, and I believe they are convincing. However, the argument that really moves me is more idealistic. By facing together what at times seems like an insurmountable challenge, we will demonstrate what is best about humanity. Ending a disease that affects people disproportionately just because of the region they live in will inspire us to be more ambitious about what is possible to achieve in our world and in our lifetime.
In recent months, vaccinators and other health workers have been targeted and killed by militants in Nigeria and Pakistan. To me, the nihilism behind these coordinated attacks—seeking out goodness to destroy it—is the opposite of what the eradication fight is about. The vaccinators were trying to stop disease and ease suffering so that even people they would never meet could have a better life.
They are heroes, and there are two ways to honor their memory: do our best to ensure the safety of those who continue the campaigns; and finish the task they gave their lives for.
I am committed to doing whatever it takes to win this fight. Ending polio is my top personal priority and the top priority of our foundation. But even the generous resources of our foundation are nowhere near enough.
The global polio community has a detailed plan for getting from here to eradication. The plan is based on a careful analysis of what countries have accomplished in the past, and what still needs to be accomplished in endemic countries in the future. This plan says that, if the world supplies the necessary funds, political commitment, and resolve, we will certify the eradication of polio by 2018.
Funds, commitment, and resolve. These are the key variables for success. If the world delivers, then we will eradicate polio within five years. It will be a remarkable success that can be added to the growing list of improvements to the human condition. We’ve cut the child mortality rate by 75 percent in the past five decades. We’ve cut the poverty rate by 50 percent in the past two decades. We’ve eradicated smallpox. These are mind-boggling successes. Adding the end of polio to the list will be one of the great moral and practical achievements of our age.
Bill Gates is the chairman of Microsoft Corporation, the world’s largest computer software maker, which he founded in 1975. He launched the Bill & Melinda Gates Foundation in 2000 to support philanthropic initiatives in the areas of global health and learning. The Foundation has since dispersed $26.1 billion in more than one hundred countries focusing on endeavors such as expanding childhood immunization, providing microfinance for small farmers, and supporting college education. In developing countries, it concentrates on improving people’s health and giving them the chance to lift themselves out of hunger and extreme poverty. In the United States, it seeks to ensure that all people—especially those with the fewest resources—have access to the opportunities they need to succeed in school and life. On Twitter: @BillGates.



